|
This article intends to provide readers with the most relevant and up-to-date information regarding the diagnosis and treatment of NTOS. This comprehensive literature review focuses on the classification, etiology, clinical presentation, diagnostic measures, and treatment of NTOS, including nonoperative therapies such as physical modalities, pharmacological therapies, minimally invasive therapies including intramuscular botulinum toxin, and surgical interventions. In addition to the controversy surrounding the diagnosis of NTOS, the treatment of NTOS also lacks consensus. 7, 9 Interestingly, even these incidences are disputed, with a more recent study analysis suggesting that NTOS may be considered a “rare” disorder, with an incidence of 2–3/100,000 per year. This lack of consensus and poor physician awareness (and therefore recognition) make it difficult to estimate the true incidence of TOS, 7 though several articles report an incidence of 3–80/1,000, 8 while Roos describes an incidence of 0.3 and 2%. 6 Further, no definitive test exists for TOS, which may suggest that TOS is relatively underdiagnosed. 5 Unfortunately, because there is a wide spectrum of presenting symptoms, there are no uniform criteria for diagnosis, treatment, patient selection, or treatment approaches. For example, the impact matches those suffering from chronic heart failure. NTOS symptoms can range from mild to severe however, if left untreated, NTOS is associated with significant detrimental impacts on functional status and quality of life. Neurogenic thoracic outlet syndrome (NTOS) can present with a wide variety of symptoms including ipsilateral upper extremity pain, sensory loss, paresis, edema, shoulder and neck discomfort, and even sympathetic nervous impairment. 3, 4 TOS can be further subclassified based on whether the etiology involves the vasculature (e.g. venous or arterial) or the brachial plexus (e.g. Three areas of compression likely exist: scalene triangle, costoclavicular space, or the pectoralis minor space. 2 The most vulnerable structures to compression are generally understood to be the brachial plexus and the subclavian vessels. 2 Some of these prior terms include “cervical rib and band syndrome”, “scalenus anticus syndrome,” and “pectoralis minor syndrome”. 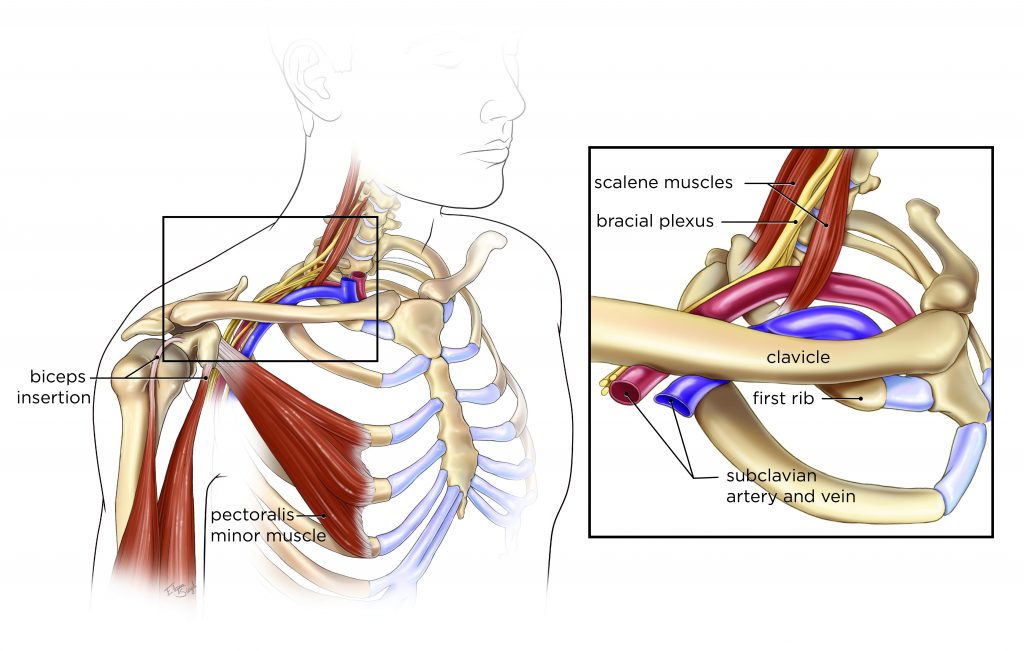
This group of disorders with a presumed compressive or nerve entrapment etiology has been described by multiple terms that reflect either the region of pathology or the maneuver that precipitated the symptoms. The term “thoracic outlet syndrome” (TOS) was coined in 1956 by Peet et al 1 and is used to describe compression of one or several neurovascular structures (ie brachial plexus, subclavian artery or vein or axillary artery or vein) that cross the thoracic outlet.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
